|
Varicose veins are swollen and enlarged veins that usually occur on the legs and feet. They may be blue or dark purple, and are often lumpy, bulging or twisted in appearance. These abnormal veins typically do not cause any problems.
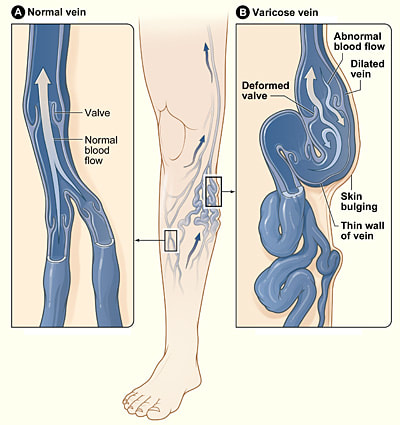
There are usually no symptoms, however some persons may experience: discolored skin in the area around the vein, itchy and thin skin over the affected vein, swollen feet and ankles, burning or throbbing in the legs. Heaviness and muscle cramps may be felt also. In worst cases, varicose veins could even cause skin ulcers, blood clots and inflammation of the veins in the legs; these require timely medical treatment. The symptoms are usually worse during warm weather or if you have been standing up for long periods of time. They may improve with walking or if you rest and raise your legs. CAUSES Varicose veins develop when the small valves inside the veins stop working properly. Normally (in a healthy vein), blood flows smoothly in one direction to the heart. The blood is prevented from flowing backwards by a train of tiny valves that open and close to let blood through. If the valves weaken or become damaged, then blood can flow backwards and collect in the vein, eventually causing it to become swollen and enlarged. (See image below) Risk factors for developing varicose veins include:
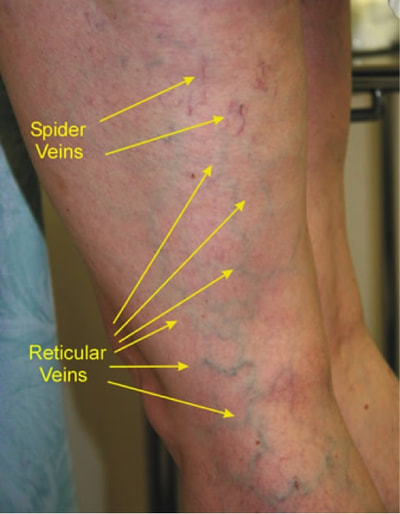
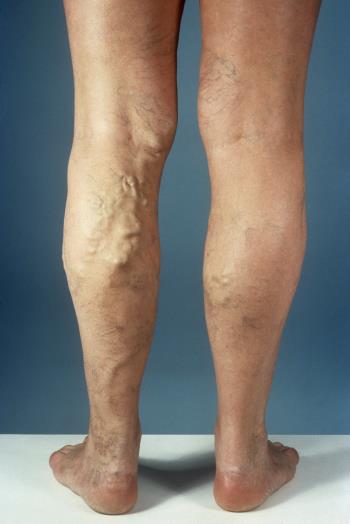
TYPES OF VARICOSE VEINS (see images below) Spider veins (also called Telangiectasia) These are blue or red veins that are very small, measuring around 0.5 to 1mm in diameter. They are harmless and can occur any where on the skin including the face. Reticular varicose veins These may be grouped close together in a network. They are deeper veins, slightly bigger (measuring 1 to 3mm diameter) and are commonly blue in color. Trunk varicose veins These are much larger veins, which are thick, long and lumpy and can often look unpleasant. TREATMENT COMPRESSION STOCKINGS Compression stockings (or socks) may first be recommend for up to 6 months, along with regular exercise and elevation of the legs when resting. These stockings exert pressure on the ankles and legs compressing the surface veins; this helps the valves to function properly and prevents back flow of blood. RADIOFREQUENCY AND ENDOVENOUS LASER ABLATION These methods involve passing a probe through the skin into the varicose vein, using ultrasound to guide the position. A device at the tip of the probe uses laser or radiofrequency energy to heat up the inside of the vein and close it off. SCLEROTHERAPY This uses a liquid/chemical that is injected into the vein to cause irritation and scarring inside, which eventually closes it off. This procedure is often used to treat smaller varicose veins and spider veins, and may require several treatments to completely close the vein off. SURGERY Surgery (Vein stripping and ligation) is normally done as a last resort or in severe cases of varicose veins. The procedure involves tying shut and removing the veins through small cuts in your skin. It is done as an outpatient procedure and the recovery time is about 1 to 4 weeks. Tip#1: Avoid standing or sitting still for long periods. Take regular breaks throughout the day and try to move around. If you need to sit or stand for a long period of time, flexing (bending) your legs occasionally can help keep blood circulating. Tip#2: Elevate the legs often above the level of your heart about 3 or 4 times a day for about 15 minutes at a time. If you have mild to moderate varicose veins, elevating your legs can help reduce leg swelling and relieve other symptoms. Tip#3: Exercise regularly; this can improve circulation and help maintain a healthy weight. Weight loss may result in significant improvement of varicose veins. Tip#4: Avoid wearing tight clothes, especially those that are tight around your waist, groin (upper thighs), and legs. Tight clothes can restrict blood flow and may make varicose veins worse. Tip#5: Avoid wearing high heels for long periods. Lower heeled shoes can help tone your calf muscles, which can help to improve blood flow in the veins. Tip#6: Wear compression stockings if you have large varicose veins. They can be effective if worn everyday, especially on days when you would be standing for very long periods. Putting them on early at mornings right after getting out of bed and removing them just before bedtime may see substantial improvement in symptoms. I hope these tips on VARICOSE VEINS were helpful; Remember, YOUR HEALTH IS INVALUABLE. By Dr. J. Lawarna Matthew Acknowledgements National Heart, Lung and Blood institute Mark O’Donnell vascular surgery (for image) St. Bartholomew Hospital/ Science photo library (for image) Visit https://www.nhlbi.nih.gov/health-topics/varicose-veins for more information.
0 Comments
Leave a Reply. |
AuthorDr. J. Lawarna Matthew Archives
January 2021
Categories |
 RSS Feed
RSS Feed
